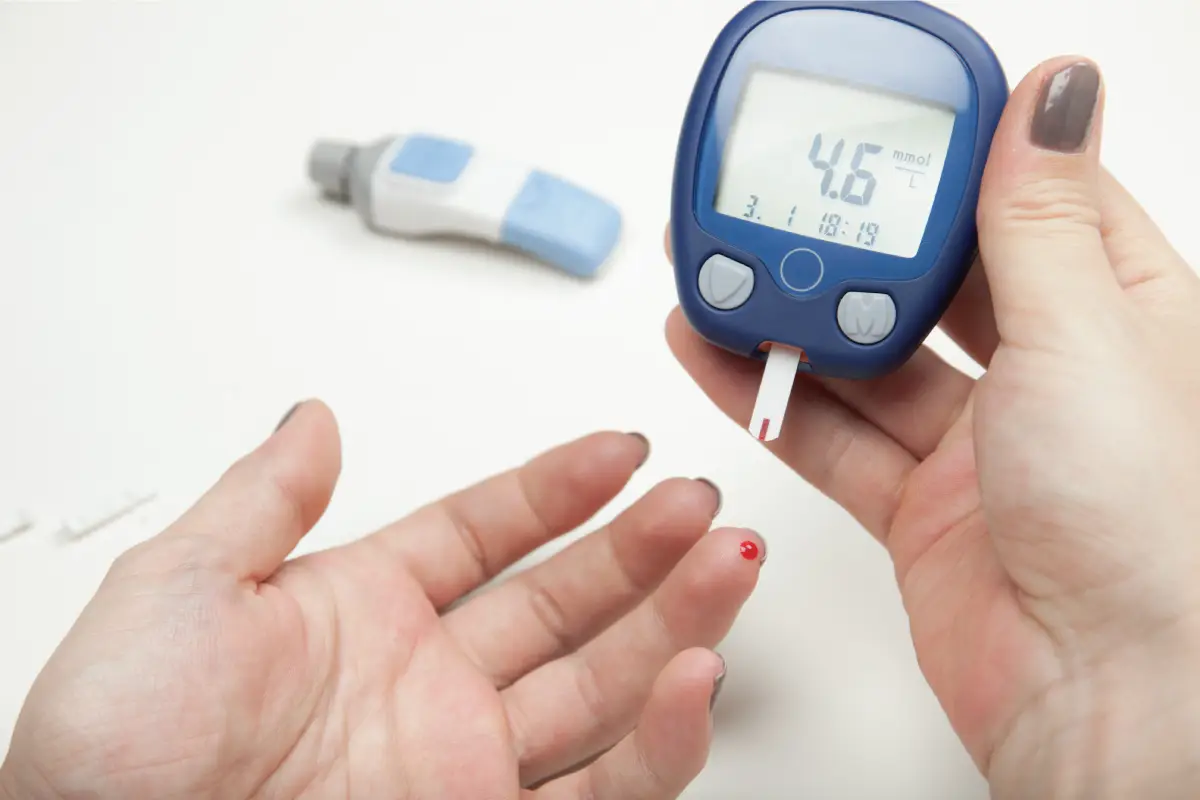
Diabetes and oral health have a powerful two-way connection. High blood sugar feeds harmful bacteria, reduces saliva flow, weakens your immune response, and slows healing.
At the same time, inflamed or infected gums release inflammatory chemicals into your bloodstream that make insulin less effective — potentially raising your A1C levels.
At Alta Loma Dental Care in Rancho Cucamonga, we’ve helped hundreds of local patients in Alta Loma, Upland, Fontana, and Ontario break this cycle with practical, personalized care. This comprehensive guide was written specifically for you. Inside you’ll discover exactly how diabetes affects your mouth, the most common oral problems to watch for, warning signs you should never ignore, the best daily oral care routine for diabetics, smart nutrition choices that support both conditions, and exactly what to expect at every dental visit. Your smile and your blood sugar are more connected than you think — let’s protect both starting today.
1. Why Diabetes and Oral Health Are Connected
If you have diabetes, your mouth is one of the first places to show signs of trouble — even before you notice other symptoms. Diabetes and oral health have a two-way relationship. This means:
- High blood sugar damages your gums and teeth
- Unhealthy gums make your blood sugar harder to control
This connection is not just a theory. The Centers for Disease Control and Prevention (CDC) and the American Dental Association (ADA) both confirm it. In fact, the ADA considers periodontal (gum) disease the sixth major complication of diabetes — right alongside heart disease, kidney disease, and vision problems.
Understanding this link is the first step toward protecting both your smile and your overall health.
Have questions about your dental health? Call us at (909) 987-6268 or Request an Appointment.

2. How Diabetes Harms Your Mouth
When blood sugar stays high for a long period, several things happen inside your mouth:
More Harmful Bacteria
High glucose in your saliva feeds the bacteria that cause plaque and tartar. More bacteria means faster gum disease. A patient who might take years to develop gum disease without diabetes can develop it in months if blood sugar is poorly controlled.
Weaker Immune System
Diabetes reduces the ability of your white blood cells to fight infection. A small cut on your gum that would heal in a few days for someone without diabetes may take weeks for you — and is more likely to become infected.
Dry Mouth (Less Saliva)
Saliva is your mouth’s natural defense system. It washes away food, neutralizes acid, and fights bacteria. High blood sugar reduces saliva production, leaving your mouth dry and at much higher risk for cavities and infections.
Slower Healing
Elevated blood sugar damages small blood vessels, reducing blood flow to your gum tissue. This means that after any dental procedure — or even a minor mouth injury — healing takes longer and infection risk is higher.
3. How Gum Disease Makes Diabetes Worse
This is the part many patients don’t know about: gum disease doesn’t just stay in your mouth.
When your gums are infected, they release inflammatory chemicals called cytokines into your bloodstream. These chemicals interfere with how insulin works in your body — making it harder for your cells to absorb glucose. The result? Your blood sugar goes up, even if your diet hasn’t changed.
Research shows that untreated gum disease can raise A1C levels by 0.4 to 1.0%. For someone trying hard to manage their diabetes, that’s a significant obstacle — one that a dentist can help remove.
The good news: treating gum disease can lower your A1C. Studies confirm that periodontal treatment (deep cleaning) can reduce A1C by 0.3 to 0.4% within three to six months. That may not sound like much, but in diabetes management, even small improvements make a real difference in preventing long-term complications.
4. Common Oral Problems in Diabetic Patients
People with diabetes are more likely to experience the following oral health problems:
Periodontal (Gum) Disease
This is the most serious oral complication of diabetes. It starts as gingivitis — red, swollen, or bleeding gums — and can progress to periodontitis, which destroys the bone holding your teeth in place. Without treatment, it leads to tooth loss.
People with diabetes are 2 to 3 times more likely to develop severe gum disease than those without diabetes.
Dry Mouth (Xerostomia)
Dry mouth affects an estimated 50 to 80% of people with diabetes. Without enough saliva, cavities form faster, and the tissues of your mouth become sore and irritated. Dentures or retainers become uncomfortable. Infections are more common.
Oral Thrush (Fungal Infection)
Thrush is a yeast infection that causes white or red patches inside the mouth. High blood sugar creates the ideal environment for yeast to grow — especially under dentures or in people who use inhaled steroids.
Slow Healing and Frequent Infections
After tooth extractions, gum surgery, or even a small bite on the inside of your cheek, healing takes much longer. Any opening in the tissue is also more likely to become infected.
Cavities
High sugar in saliva, reduced saliva production, and a weakened immune system combine to make cavities far more common in diabetic patients. Patients with poorly controlled diabetes are three times more likely to lose teeth than those with well-managed blood sugar.
5. Warning Signs You Should Never Ignore
Contact Alta Loma Dental Care right away if you notice any of the following:
- ✅ Gums that bleed when you brush or floss
- ✅ Red, swollen, or tender gum tissue
- ✅ Gums that seem to be pulling away from your teeth
- ✅ Teeth that feel loose
- ✅ Persistent bad breath that doesn’t go away with brushing
- ✅ Constant dry mouth, even when you drink plenty of water
- ✅ White patches or sore red areas in your mouth (possible thrush)
- ✅ Mouth sores that haven’t healed within two weeks
- ✅ A burning feeling in your mouth or on your tongue
- ✅ Changes in how your food tastes
Early treatment is always easier, faster, and less expensive than treating advanced problems. Don’t wait.
6. Your Daily Oral Care Routine for Diabetes
The good news: most diabetes-related oral problems are preventable with the right daily habits. Here is a simple, effective routine that works well for our Rancho Cucamonga patients.
Morning Routine
- Brush for 2 full minutes using a soft-bristled toothbrush and fluoride toothpaste (look for the ADA Seal of Acceptance).
- Floss between every tooth. If gums bleed at first, keep going gently — this usually improves within a week or two as the gum health improves.
- Rinse with an alcohol-free antibacterial mouthwash. Alcohol-based rinses can make dry mouth worse.
- Check your blood sugar and make sure it’s in your target range before eating.
- Drink a glass of water to stimulate saliva flow.
Evening Routine
- Brush again before bed, especially after your last meal or snack.
- Floss thoroughly — this is the most important flossing session of the day, as bacteria are most active overnight.
- Apply any prescribed fluoride gel if your dentist has recommended one.
- Sip water — avoid sugary drinks at night.
Managing Dry Mouth at Home
- Sip water throughout the day — keep a bottle with you at all times.
- Chew sugar-free gum to stimulate saliva.
- Use a bedroom humidifier at night if you sleep with your mouth open.
- Ask your dentist about over-the-counter saliva substitutes (such as Biotene) or prescription options if dry mouth is severe.
- Avoid alcohol, caffeine, and tobacco — all of which worsen dry mouth.
Products That Help
- Electric toothbrush: Significantly more effective than manual brushing for removing plaque
- Water flosser (Waterpik): Great for patients who struggle with traditional floss
- Dry-mouth toothpaste and rinse: Biotene or similar alcohol-free products
- Fluoride varnish: Applied in-office at Alta Loma Dental Care every 3 to 4 months for high-cavity-risk patients
7. What to Eat (and Avoid) for Healthy Teeth and Blood Sugar
What you eat affects both your blood sugar and your oral health at the same time. The right food choices can protect your teeth and help stabilize your glucose levels simultaneously.
Foods That Support Both Diabetes and Oral Health
| Food | Why It Helps |
|---|---|
| Crunchy vegetables (carrots, celery, bell peppers) | High fiber slows blood sugar spikes; natural scrubbing action cleans teeth |
| Leafy greens (spinach, kale) | Low glycemic index; high in calcium and vitamin C for gum health |
| Fatty fish (salmon, sardines) | Omega-3s reduce gum inflammation; vitamin D supports strong teeth |
| Nuts and seeds (almonds, walnuts, chia) | Minimal blood sugar impact; magnesium improves insulin sensitivity |
| Plain Greek yogurt and cheese | Calcium and phosphorus strengthen enamel; probiotics may reduce harmful oral bacteria |
| Green tea (unsweetened) | Polyphenols reduce inflammation and bacterial growth; zero blood sugar impact |
| Water | Rinses away food and bacteria; stimulates saliva production |
Foods to Limit or Avoid
| Food | Why It’s Problematic |
|---|---|
| Sticky dried fruits (raisins, dates) | Cling to teeth and contain concentrated natural sugars |
| Sugary sodas and juice | Feed oral bacteria and spike blood sugar |
| Diet sodas | Acidic; erode tooth enamel even without sugar |
| White bread and crackers | Quickly convert to sugar, feeding bacteria |
| Candy and sweets | Obvious risk for both blood sugar and cavities |
Many patients at our Rancho Cucamonga practice report that eating more of these diabetes-friendly foods noticeably reduces gum bleeding and morning dry mouth within a few weeks.
📋 For more nutrition guidance tailored to dental health, visit our Nutrition Tips for Healthy Teeth and Gums patient resource.
8. How Often Should People With Diabetes See a Dentist?
The general recommendation is at least twice a year (every 6 months) for a professional cleaning and exam. However, many dental and medical organizations — including the American Diabetes Association — recommend that patients with diabetes be seen every 3 to 4 months, especially if:
- You have active gum disease
- Your A1C is above 7%
- You experience frequent dry mouth
- You have had recent dental infections or slow healing
More frequent visits are not just about cleaning your teeth — they allow your dental team to catch problems early, when they are easiest (and least expensive) to treat.
Before Your Dental Appointment: What to Do
- Eat normally and take your medications on schedule — do not skip meals before your visit
- Bring your medication list, including insulin type and dosage if applicable
- Bring your most recent A1C result so we can tailor your treatment plan
- Tell us if your blood sugar has been harder to control recently
During the Appointment
- Let us know immediately if you feel lightheaded, shaky, or sweaty — these can be signs of low blood sugar
- We may check your blood glucose with a glucometer before procedures if you are on insulin
9. What to Expect at Alta Loma Dental Care
At Alta Loma Dental Care, we take diabetes and oral health seriously — because we know how much one affects the other.
Here’s what your first comprehensive diabetic oral health visit looks like:
Step 1: Medical and Dental Review
We’ll review your diabetes history, current medications, recent A1C levels, and any oral symptoms you’ve noticed. This helps us understand the full picture before we look at your mouth.
Step 2: Thorough Oral Exam
We measure gum pocket depths (a key indicator of periodontal health), check for signs of dry mouth and thrush, screen for oral cancer, and evaluate every tooth for cavities and wear. We take X-rays as needed to see what’s happening below the gum line.
Step 3: Professional Cleaning
Our hygienists are trained in gentle, thorough cleaning techniques especially suited for patients with sensitive or inflamed gums. If there are signs of periodontal disease, we discuss scaling and root planing (deep cleaning) — the most effective non-surgical treatment for gum disease, which research confirms can lower A1C levels.
Step 4: Personalized Care Plan
We create a custom treatment and maintenance plan based on your specific type of diabetes, current A1C, medications, and oral health status. We also coordinate care with your primary care physician or endocrinologist when needed.
Step 5: Ongoing Support
We are here between appointments too. If you notice new symptoms — bleeding, swelling, a sore that won’t heal — call us at (909) 987-6268. We offer same-day appointments for urgent concerns.
We serve patients throughout Rancho Cucamonga, Alta Loma, Upland, Fontana, and Ontario.
10. Type 1 vs. Type 2: Are There Differences in Oral Health?
Both types of diabetes affect your mouth through elevated blood sugar, but there are some important differences to know.
Type 1 Diabetes and Oral Health
- Oral problems can appear earlier in life, since Type 1 often begins in childhood
- Hypoglycemia risk during dental appointments is higher — always tell us your insulin schedule and blood sugar level before treatment
- Children with Type 1 may experience delayed tooth development if blood sugar is poorly controlled during growth years
- Insulin pumps and continuous glucose monitors should generally stay on during dental visits — confirm with your endocrinologist
Type 2 Diabetes and Oral Health
- Many Type 2 patients have had elevated blood sugar for years before diagnosis, so gum disease may already be present when diabetes is first identified
- Common Type 2 medications (including metformin) can cause dry mouth — be sure to share your medication list with us
- The systemic inflammation linked to excess weight compounds gum inflammation, often making periodontal disease more severe
- Some patients who achieve significant weight loss and blood sugar control experience dramatic improvements in gum health, sometimes reversing early-stage gum disease entirely
What Both Types Have in Common
Regardless of which type you have, the essential steps are the same:
- Keep your A1C within your target range (typically below 7%)
- Brush and floss every day using the correct technique
- Visit Alta Loma Dental Care every 3 to 6 months
- Report any new oral symptoms promptly
- Keep your dentist and your diabetes care team in communication
This article about oral health and diabetes is for informational purposes only and does not substitute professional dental or medical advice. Always consult with your dentist and physician regarding your specific health conditions.